What an anesthesiologist wants you to know before surgery
Plus: What are “tendons”? + Find a food bank in your community.
Welcome to Doing Well. Today:
Word of the week: tendon
Health news we’ve found useful this week
Where to find a food bank in your community
Thanks for reading—let’s get started.
We Asked: What should we know about anesthesia?
Every day about 60,000 people—enough to fill the Arizona Cardinals’ football stadium—have surgery under general anesthesia. By temporarily blocking the signals between your nerves and your brain, anesthesia helps patients get through medical procedures that would otherwise be impossible.
Anesthesia often happens behind the scenes, and patients have a less direct relationship with their anesthesiologist than they do with other doctors. Anesthesia can also be scary for patients—while it’s a safe, routine, and vital part of our medical system, as is the case for all medications, there are side effects and risks. Because not everyone reacts the same to anesthesia, administering anesthesia is a complex and evolving science.
To learn more about how anesthesia works and the conversations you can have with your doctor about it, we spoke to Dr. Steve Dentz, an anesthesiologist and assistant professor of clinical practice at ASU’s John Shufeldt School of Medicine and Medical Engineering. Our conversation has been edited for length and clarity.
Short on time? Here’s what to know:
The job of an anesthesiologist is to help keep a patient comfortable during a medical procedure. They administer medications and monitor vital signs, ensuring a procedure is as safe and painless as possible.
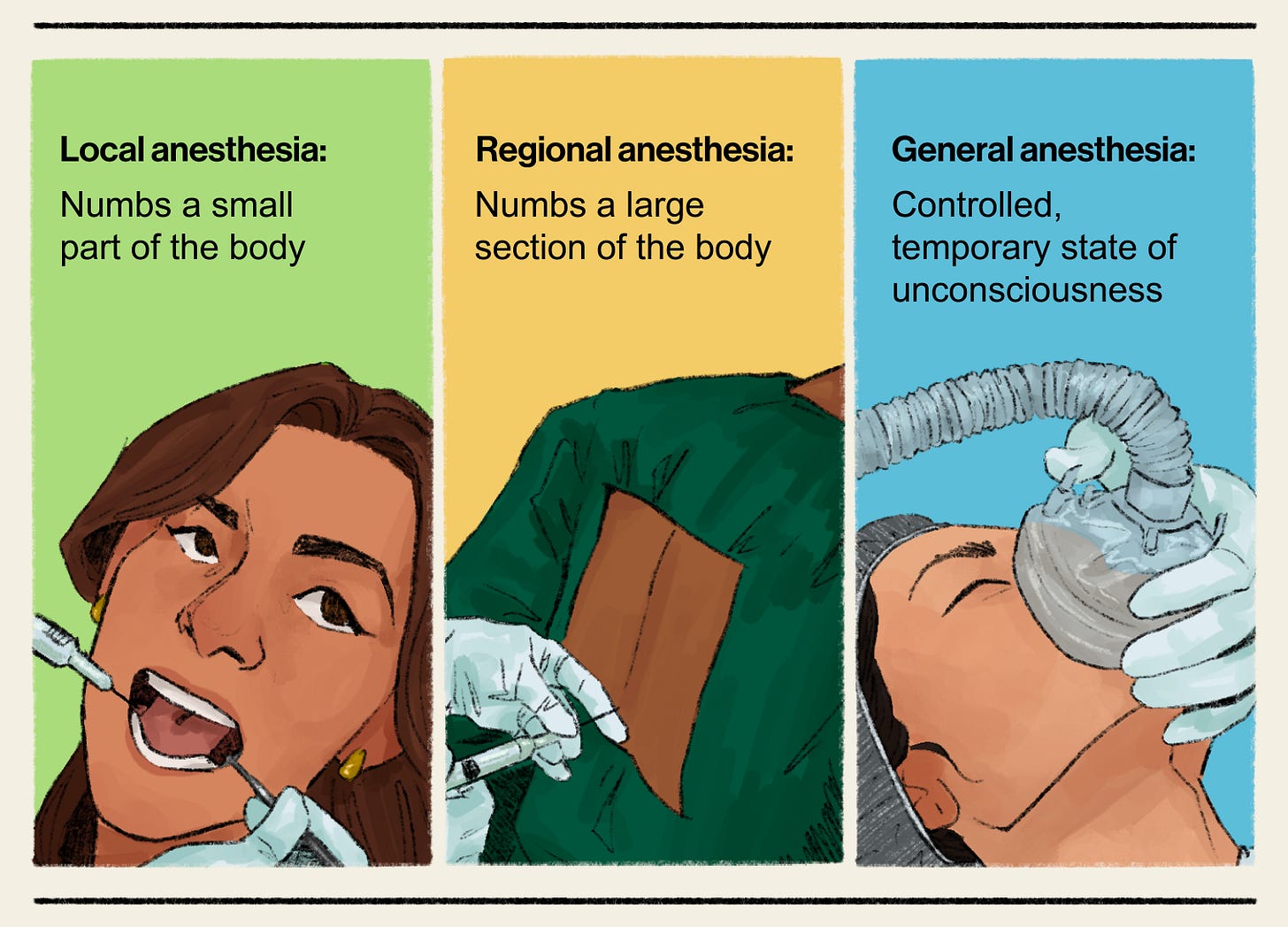
There are three types of anesthesia: general, regional, and local. General anesthesia is used for procedures where the patient needs to be totally asleep—for example, heart surgery. Regional anesthesia numbs a large part of the body while a patient stays awake—for example, through an epidural during labor. Local anesthesia numbs a smaller part of the body—like your mouth during a cavity filling—and usually doesn’t require an anesthesiologist. Anesthesiologists can also give sedation medicine, which helps someone relax and feel sleepy.
Before a procedure that involves anesthesia, you can ask your doctor to walk you through the anesthesia plan and address any concerns you have. For example, nausea is a common side effect of anesthesia that can be addressed through medication—you can ask your anesthesiologist how they plan to do so.
People react differently to anesthesia, which means anesthesiologists have to continuously monitor how a patient is doing and adjust the medications they’re giving as needed. Genetics may impact your reaction to anesthesia, but research is still ongoing to understand how.
Mia Armstrong-López: In broad strokes, what is the job of an anesthesiologist?
Steve Dentz: We accompany a patient to the operating room and see them safely through the process. The surgeon is going to focus on fixing whatever the issue is that required that patient to go to the operating room. As anesthesiologists, we’re managing everything that isn’t that piece of the surgery. We’re getting the patient off to sleep, administering medicines so that they’re waking up feeling as pain-free or as comfortable as possible. We’re making sure that their blood pressure and heart rate stay within a safe range. We’re managing the other medical pieces.
MAL: There are different types of anesthesia, administered both inside and outside the operating room. What are the different categories of anesthesia?
SD: We primarily break it down into three categories. The first category would be general anesthesia—any time that we’re specifically giving patients medicines to have them go off to sleep completely for the surgery.
The second would be regional anesthesia. We think about that more along the lines of somebody that gets a spinal anesthetic, which is an injection of anesthesia medicine through the skin of somebody’s lower back, and that medicine numbs up their body from their belly button down to their toes. We could do that, say, for somebody having hip replacement surgery or knee replacement surgery. Another category under regional anesthesia would be when we place an epidural catheter for a woman that’s in labor and desiring pain relief. With an epidural, we leave a small plastic tube in place, about the size of a piece of wet spaghetti. And that tube acts as a means by which we can give medicine the entire time she’s in labor to help with pain relief.
The third category would be local anesthesia. As anesthesiologists, that’s not typically what we’re doing. Local anesthesia lends itself better when surgeons are doing small procedures in their office, where they can just numb up a little area.
Something that can go along with local or regional anesthesia would be additional sedation medicines. Not quite to the level of general anesthesia, where somebody is 100% asleep—but some sedation that would make somebody kind of sleepy but easily arousable. Providing sedation might be a layer that we add on top of something else.
MAL: When you talk to patients about anesthesia, what are their most common concerns?
SD: The biggest thing is general nervousness or anxiety about needing to go to the operating room. We don’t meet people a whole lot prior to being in the pre-op area right before the surgery’s going to start. They don’t always have a lot of time to think about the anesthesia. The most common thing is just sort of general anxiety about what the anesthesia plan will be to get them off to sleep or comfortable for the surgery.
If people have been through anesthesia before, they may have some more specific concerns. Nausea after anesthesia and after surgery is still fairly common; that’s one of the bigger complaints to address, telling that patient ahead of time how we’ll try to deal with it. Specific to the anesthesia plan, there can be a lot of anxiety thinking about having a needle put in their back. Those are probably the three biggest things: General anxiety about needing to go to the operating room, concerns about nausea if they’ve been through it before, and some specific things related to an anesthetic plan.
MAL: What options are you able to offer patients with those concerns?
SD: Specific to nausea, I will let them know that they’ll be receiving anti-nausea medicines. It’s pretty common for me to administer two different medicines to help prevent nausea afterwards. What I always tell them is: I’ll be giving you two medicines to help prevent nausea. They’ll be given to you through your IV while you’re asleep during the surgery, and they work good alone, but they work even better in combination. For patients that have general anxiety about heading to the operating room, simply talking in the pre-op area—letting them know that I and the entire team are all going to work very hard to make this go as smoothly as possible for you, really reiterating to them that everyone is here to focus on them and make this go as safely as possible and smoothly as possible—can often help.
MAL: What does the process actually look like for you in the operating room? What are you paying attention to?
SD: It’s a pretty high-tech field between the anesthesia machine and the monitors that we use to monitor vital signs. I describe it once we’re in the operating room and I’m hooking up those monitors, because I like to let the patient know everything I’m doing—I don’t like for my actions to catch them off guard. What we use for everyone is a monitor to keep an eye on the electrical activity of their heart, for any funny heart rhythms or anything like that. We’ll put a blood pressure cuff on, and we usually set it so that it’s checking their blood pressure every three minutes for the entire duration of the surgery, so we can keep a close eye on any changes. An additional monitor we use is called a pulse oximeter, it tells us how much oxygen is being carried by our red blood cells.
We usually monitor somebody’s temperature while they’re in the operating room. General anesthesia can cause problems with the body’s ability to auto-regulate its temperature—the tendency is for somebody’s core temperature to drop during the course of surgery. So we’ll keep an eye on their temperature, and we have warming blankets and other things to offset that. With general anesthesia, a lot of times we’ll put a breathing tube in for the duration of the surgery. The breathing tube only goes in once the patient is asleep and typically comes out at the end of the surgery before they’re awake enough to even know that it was there. When the breathing tube is in place, it allows us to breathe for the patient when they’re too deep under anesthesia to do that on their own. One of the things we can monitor with the breathing tube in place is the amount of carbon dioxide that the patient is breathing out with each breath [and] the number of times that the person is breathing per minute.
MAL: Different bodies react differently to medications, and so part of your job is figuring out what level of medication is needed for the particular patient in front of you. What factors affect how people respond to anesthesia?
SD: We don’t know everything about how different people respond differently to medicines. In the anesthesia community, we know there can be great variability. We know that people with red hair can actually have higher anesthetic requirements. They can still have anesthesia safely, they just sometimes require more medicine than somebody else might.
When I’m talking to patients and they ask, How do you know how much to give?, I say, Well, we often use somebody’s weight as a starting point, but there is no fixed answer. Anesthesia sometimes is like a recipe. It’s like a recipe for chili, because there’s a lot of things that go into it. There are medicines to go to sleep. There are medicines to help make sure you don’t wake up having too much pain. There are medicines to help prevent nausea. There are medicines to help relax your muscles. We use lots of different things. We may start with a basic recipe, but just like a good chef, you always want to see if you need to add something else. So weight is our starting point, that’s the science. The art is being able to respond exactly to you—observe you, see how you are doing, and then add what we need to to make sure that you’re where we need you to be.
MAL: What goes into your assessment of what needs to be adjusted?
SD: Even under general anesthesia, we can look at vital signs as an overall gauge. As an example, if we see that their heart rate goes up and their blood pressure rises, those can be indications that we need to increase the level of anesthesia for whatever the surgeon might be doing at that moment in time. So even though they may not be able to talk to us, part of what comes from being a seasoned clinician and taking care of enough patients is using those other vital signs as surrogates of something that’s changing during the operation, where we might need to then change the anesthetic.
MAL: It’s powerful as a patient, this idea that there’s someone who’s specifically tuned in to your comfort and your needs, even when you can’t be actively voicing them.
You’ve been practicing for almost three decades. What is the most exciting way that technology has changed your field over that time?
SD: Something I’ve seen evolve is the use of ultrasound in anesthesia. I can give you an example. Throughout the entire duration of my practice, I’ve done something called nerve blocks, where we can administer local anesthesia around certain nerves to try to provide pain relief after different types of surgeries. When I first started, we used a little device that we connected to an insulated needle, and it delivered a tiny electrical pulse. Boom, boom, boom. When the tip of that needle would get close to the nerve, it would make the muscles in the patient’s arm twitch, so we knew we were where we wanted to be.
These days, though, I don’t use that at all. I use an ultrasound probe on the patient’s neck. An ultrasound uses painless sound waves to see inside the human body, so I can use the ultrasound probe to visualize inside the neck, see that nerve bundle, and then help guide the needle to right where I want to put the local anesthesia.
MAL: It’s like driving with GPS.
SD: Right. We used to have to unfold the map at home on the kitchen table before we went somewhere. Now we can plug in an address, and it guides us right to where we want to go.
Well-Informed: Related stories from the ASU Media Enterprise archives
What’s the history of anesthesia? In this article for Zócalo Public Square, Virginia Wright-Peterson writes about Alice Magaw, a nurse who helped set the “national standard” for administering anesthesia. Dubbed the “mother of anesthesia,” Magaw worked at the hospital that would evolve into the Mayo Clinic. She administered 14,000 anesthetics without a single anesthesia-related death—a feat at the time—and published about her techniques in medical journals for other health care providers to consult.
Well-Versed: Learning resources to go deeper
How does your body send signals from your nerves to your brain? Learn all about it in this edition of ASU’s Ask a Biologist on the nervous system.
Well-Read: News we’ve found useful this week
“Health influencers are all over social media. How to be smarter when vetting claims,” by Devi Shastri, May 9, 2026, Associated Press
“I saved $800 on my medical bills with an easy trick,” by Alex Olgin, April 25, 2026, Slate
“8 health insurance terms you should know,” by Jackie Fortiér, May 11, 2026, KFF Health News
Well-Defined: Word of the week
Bones, muscles, and tendons work together to move your body.
But what is a tendon? A tendon is like a strong “rope” of tissue that connects muscle to bone. As a muscle squeezes, the tendon pulls on the bone, which allows for movement.
Tendons can be found throughout the body, from head to toe. To keep your tendons healthy, it’s important to warm up before you exercise, stretch after exercise, and balance different types of movement, among other recommendations.
-Kitana Ford, health communication assistant
Well-Engaged: Food access in your community
In the U.S., an estimated 1 in 7 people experiences food insecurity—a fact that is both tragic and preventable.
There are many reasons someone might have a hard time accessing food: making a wage that doesn’t match the cost of living, being unable to get to the grocery store, losing a job or being unable to work, among many other barriers. Food insecurity is the result of big, systemic problems, not individual choices.
Public food assistance programs can help people facing food insecurity, but not everyone will meet their requirements. Food banks help fill the gaps. Whether you need food resources or would like to find ways to donate, here’s a list of organizations you can reach out to:
Local resources:
National resources:
Child resources:
Looking for resources in an area where food banks are hard to find? Locate a mobile pantry near you. If you are a senior in need, locate a senior food program near you.
-Kitana Ford, health communication assistant
Do you have a question or topic you’d like us to ask an expert about? We want to hear from you.